Refractive Lens Exchange: Definition, Process, & Recovery
As we get older, changes in our vision can gradually disrupt the clarity we once took for granted. Reading fine print, focusing at arm’s length, or seeing clearly across different distances may all become more challenging. For those seeking a long-term approach to vision correction, especially when laser eye surgery isn’t suitable, refractive lens exchange offers a compelling alternative.
In this article, we’ll explore how refractive lens exchange works, who may benefit from it, and what to expect from the process so you can decide if it’s the right next step towards clearer, more comfortable vision.
What Is Refractive Lens Exchange?
Refractive lens exchange (RLE), sometimes known as lens replacement, is a surgical procedure during which the eye’s natural lens is replaced with a better-functioning intraocular lens (IOL). This is done to correct refractive errors and reduce dependence on glasses or contact lenses.
Although the procedure is nearly identical to cataract surgery, RLE is performed before the lens becomes cloudy. It’s often chosen by people who want a permanent solution to vision issues, especially when they’re not suitable candidates for laser eye surgery like LASIK or PRK.
Common Refractive Errors Treated With RLE
Refractive lens exchange is designed to correct a range of vision conditions known as refractive errors, where the eye does not bend light properly, resulting in blurred or distorted vision.
Below are some of the most common types addressed with RLE:
- Myopia (Short-Sightedness): Difficulty seeing distant objects clearly. RLE can implant a lens to improve distance vision.
- Hyperopia (Long-Sightedness): Struggling with close-up tasks? An artificial lens can be tailored to restore clarity for near vision.
- Astigmatism: Caused by an irregularly shaped cornea. Toric premium lenses may help correct refractive errors linked to astigmatism.
- Presbyopia: Age-related vision loss for near tasks. RLE may provide relief through multifocal lenses or blended vision strategies.
How Refractive Lens Exchange Works
It typically begins with your surgeon creating an incision at the edge of the cornea. Through this small entry point, an ultrasound probe is used to gently soften and remove the eye’s lens.
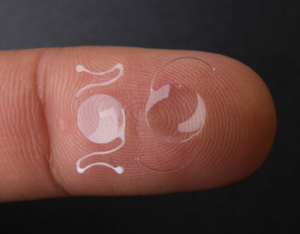
Once the original lens is removed, a carefully selected artificial intraocular lens (IOL) is inserted through the same cut and positioned securely within the lens capsule, the natural membrane that holds the lens in place.
The new replacement lens is designed to meet your specific visual requirements, helping to improve clarity at one or more distances depending on the type of lens chosen.
Understanding Your Lens Options
You’ll work with your eye doctor to choose a lens that aligns with your visual requirements and lifestyle. Options include:
Monofocal Lenses
These lenses are set for a single distance, typically the clear distance. You may still wear reading glasses for close-up tasks.
Multifocal Lenses
These are designed to provide multiple focal points, allowing for improved near vision, intermediate tasks, and distance clarity. Many people choose these to reduce their reliance on spectacles.
Accommodative Intraocular Lenses (IOLs)
Accommodative IOLs are designed to move or shift slightly within the eye, mimicking the natural focusing ability of a healthy lens. For those seeking greater visual flexibility, accommodative lenses may offer a balance between clarity and comfort, with less dependence on additional eyewear.
Recovery And Aftercare
Here’s what to expect after undergoing lens replacement:
- Eye Drops And Healing: Your doctor will prescribe eye drops to help with healing, reduce inflammation, and prevent infection. Following your aftercare plan carefully can support your recovery.
- Returning to Normal Activities: You should be able to resume normal activities within a few days. You’ll attend follow-up visits to monitor healing, lens stability, and intraocular pressure.
 Is Refractive Lens Exchange the Same As Cataract Surgery?
Is Refractive Lens Exchange the Same As Cataract Surgery?
The procedures are nearly identical in technique, but the purpose is different. Cataract surgery is performed when the natural lens becomes cloudy and impairs vision.
RLE, however, is done while the lens is still clear, hence the name clear lens exchange. It’s an elective procedure aimed at vision correction, rather than treating a medical condition.
How Other Vision Correction Methods Differ From RLE
Let’s take a closer look at how refractive lens exchange compares to other vision correction options in practical terms:
With LASIK, your cornea is reshaped to correct vision, but your natural lens stays in place. LASIK may not suit those with thin corneas or age-related vision decline.
PRK also reshapes the cornea but involves a longer healing time. Like LASIK, it doesn’t address presbyopia.
Implantable collamer lenses (ICLs) involve inserting a lens over your natural one, without removing it. ICLs are reversible, whereas RLE replaces the lens entirely and offers a more permanent solution.
Are There Risks?
Every surgical procedure carries some risks, and RLE is no exception. Though complications are rare, you should be aware of possible risks such as:
- Retinal detachment
- Glare or halos at night
- Increased intraocular pressure
- Infection
- Lens dislocation
- Posterior capsular opacification (a treatable cloudiness behind the lens)
Choosing a qualified professional and attending follow-up appointments can help monitor and address these risks early on.
Frequently Asked Questions
How long does the surgery take?
Refractive lens exchange surgery usually takes around 15 to 30 minutes. While it is relatively quick, you should allow extra time on the day for preparation, recovery, and post-operative checks before heading home.
Will lens replacement surgery hurt?
Since the eye is numbed using anaesthetic eye drops, you won’t feel much pain during the procedure.
You may notice some pressure or slight movement, but most people describe the experience as comfortable. A light sedative may also be offered to help you feel relaxed throughout.
 Can both eyes be done at the same time?
Can both eyes be done at the same time?
It depends on your personal needs and the recommendation of your eye surgeon.
Some people prefer to have both eyes treated on the same day for convenience, while others choose to space the procedures a few days or weeks apart to evaluate the result in one eye before proceeding with the other. Your surgeon will discuss the best option based on your vision, lifestyle, and preferences.
Final Thoughts
Refractive lens exchange may not be for everyone, but for many, it’s a chance to regain clearer, more comfortable vision without the daily limitations of glasses or contact lenses.
By replacing your natural lens with a carefully selected intraocular lens, RLE offers a vision correction approach that aligns with your lifestyle, preferences, and future.
If you’re ready to explore this option further, the best next step is to schedule a comprehensive eye examination with a qualified eye care professional. Your journey to long-lasting clarity may be closer than you think.
If you’re curious about how refractive lens exchange could support your long-term vision goals, we’re here to help. A personalised consultation can give you greater clarity on whether RLE is the right path for your eyes, your lifestyle, and your visual needs.
Contact our eye clinic located in Armadale Melbourne today at (03) 9070 5753 to book your comprehensive eye examination and take the first step towards clearer, more confident vision.
Note: Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
References
Rowden A. What Are Phakic Intraocular Lenses? [Internet]. Medical News Today. 2025 [cited 2025 Jul 23]. Available from: https://www.medicalnewstoday.com/articles/phakic-intraocular-lens
Chan E, Varma S. Refractive Lens Exchange – The Evidence Behind the Practise. Eye [Internet]. 2024 Nov 14;208–209(39). Available from: https://www.nature.com/articles/s41433-024-03478-3
Zimlich R. Lens Replacement Surgery: When You Might Need This Eye Procedure [Internet]. Healthline. 2022 [cited 2025 Jul 23]. Available from: https://www.healthline.com/health/eye-health/lens-replacement-surgery



 Is Refractive Lens Exchange the Same As Cataract Surgery?
Is Refractive Lens Exchange the Same As Cataract Surgery? Can both eyes be done at the same time?
Can both eyes be done at the same time?




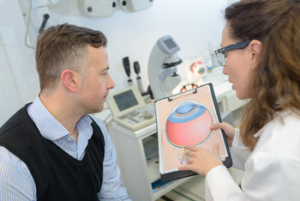 Why Are Intraocular Lenses Used?
Why Are Intraocular Lenses Used?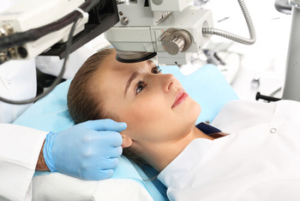 While generally successful, IOL implantation is still a surgical procedure and
While generally successful, IOL implantation is still a surgical procedure and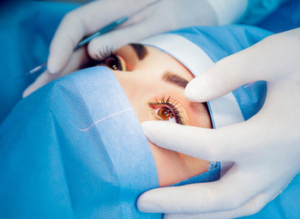 IOLs are designed to last for many years. They’re made from durable materials that do not break down or need replacement in most cases.
IOLs are designed to last for many years. They’re made from durable materials that do not break down or need replacement in most cases.


 Internal Stye
Internal Stye Antibiotics for Treating A Stye
Antibiotics for Treating A Stye
 Some people are simply prone to styes even without possessing any known risk factors. For others, there are some identifiable risk factors. These can include:
Some people are simply prone to styes even without possessing any known risk factors. For others, there are some identifiable risk factors. These can include:

 However, if the bacterial infection associated with a stye progresses to an infection of the surrounding tissues, known as preseptal cellulitis, this will require antibiotic treatment.
However, if the bacterial infection associated with a stye progresses to an infection of the surrounding tissues, known as preseptal cellulitis, this will require antibiotic treatment. 




 Treatment
Treatment

 In most cases, cataracts are associated with increasing age and are an entirely normal development. These are known as age-related or senile cataracts.
In most cases, cataracts are associated with increasing age and are an entirely normal development. These are known as age-related or senile cataracts.  Conversely,
Conversely, 
 During
During 


 A carcinoma is a type of cancer arising from epithelial tissue. These cells are found in the skin but also can line our internal organs, such as the kidneys, and also our body cavities, such as the chest cavity. There are also different types of epithelial cells, which can give rise to different types of carcinoma cancers., including sebaceous carcinoma and
A carcinoma is a type of cancer arising from epithelial tissue. These cells are found in the skin but also can line our internal organs, such as the kidneys, and also our body cavities, such as the chest cavity. There are also different types of epithelial cells, which can give rise to different types of carcinoma cancers., including sebaceous carcinoma and  Similar to squamous carcinomas of the eyelid, basal cell carcinomas are associated with lighter-skinned patients with a history of UV damage to the skin. Other risk factors include:
Similar to squamous carcinomas of the eyelid, basal cell carcinomas are associated with lighter-skinned patients with a history of UV damage to the skin. Other risk factors include:
 An unexpected cause of
An unexpected cause of