How Is Glaucoma Diagnosed? What to Know About Glaucoma Tests
Glaucoma is a group of eye diseases that can potentially lead to vision loss. But how is glaucoma diagnosed?
Understanding its diagnosis is an essential step in protecting your eye health and maintaining your quality of life. Early detection and timely management are necessary for slowing disease progression and preventing irreversible vision loss.
Understanding Glaucoma

While some types of glaucoma are associated with elevated eye pressure, other forms can occur even when eye pressure is within the normal range.
Glaucoma often progresses slowly, with minimal symptoms in the early stages. This makes regular eye examinations crucial, especially for individuals at higher risk.
Types of Glaucoma
Understanding the types of glaucoma is essential for both early detection and informed management. Each type affects the optic nerve differently, and recognising the specific form can help your eye doctor select the appropriate glaucoma test and treatment plan.
Primary Open-Angle Glaucoma
Primary open-angle glaucoma is a common form of glaucoma. It develops gradually, often without noticeable vision loss in the early stages. The optic nerve slowly sustains damage, typically affecting peripheral vision first.
Because obvious symptoms may not appear until later, regular comprehensive eye tests are crucial for early detection. Identifying this type early allows for interventions such as prescription eye drops or laser treatment to help lower eye pressure and slow disease progression.
Angle-Closure Glaucoma
Angle-closure glaucoma can appear suddenly and may be a medical emergency. Symptoms may include severe eye pain, pressure in your eye, blurred vision, headache, and occasionally nausea. Immediate assessment is essential to prevent rapid optic nerve damage and irreversible vision loss.
Early recognition and intervention, including laser surgery or other surgical procedures, can stabilise eye pressure and protect vision.
Congenital Glaucoma
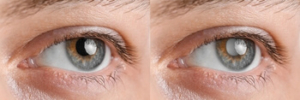
Congenital glaucoma is present at birth, caused by abnormalities in the eye’s drainage system. Infants may show signs such as cloudy corneas, dilated pupils, or light sensitivity.
Prompt diagnosis is critical for protecting eye health and supporting normal visual development. Treatments may include surgical procedures to improve fluid drainage and effectively manage pressure inside the eye.
Normal-Tension Glaucoma
Normal-tension glaucoma is characterised by optic nerve damage even when eye pressure is within the normal range. Contributing factors may include low blood pressure, a thin cornea, or other medical conditions that affect blood flow to the optic nerve.
Diagnosis often relies on visual field tests and careful monitoring rather than eye pressure tests alone. Early detection is key to developing a personalised treatment plan and slowing disease progression.
Identifying the type of glaucoma is important because it directly informs which diagnostic tests and treatment options are appropriate.
Whether managing open-angle glaucoma with prescription eye drops, addressing angle-closure glaucoma with laser surgery, or monitoring normal-tension glaucoma, understanding the distinctions enables you to actively take care of your eye health.
Risk Factors That Influence Diagnosis

- Family history of glaucoma or being a glaucoma suspect.
- Age over 40, particularly in people with thin corneas.
- Existing medical conditions, like diabetes or cardiovascular disease.
- Previous eye injuries or history of cataract surgery.
Being aware of these factors can help you and your eye doctor prioritise early detection and timely management.
The Role of a Comprehensive Eye Exam
A detailed eye exam is a key step in understanding how glaucoma is diagnosed. During such an exam, an eye doctor may evaluate several aspects of eye health. These assessments help identify potential signs of optic nerve damage or vision changes, which are important for monitoring disease progression.
Regular eye examinations allow for observation of changes over time. This ongoing monitoring can support early detection and help guide appropriate treatment options before significant vision loss occurs.
Measuring Eye Pressure
Assessing intraocular pressure is often one of the first considerations in a glaucoma assessment. Elevated intraocular pressure can indicate a higher risk of optic nerve damage, though high pressure alone does not confirm a diagnosis.
An eye doctor may use different approaches to estimate eye pressure, and the findings can inform whether additional evaluation or monitoring is needed.
Examining the Optic Nerve
Evaluating the optic nerve can provide insight into possible early signs of glaucoma. Some methods allow doctors to view the optic nerve more closely or track subtle changes over time.
This can help understand how the condition might be progressing, even if vision loss is not yet noticeable.
Assessing Peripheral Vision
Checking peripheral vision can indicate early areas of vision loss. Changes in side vision or the development of blind spots may reflect optic nerve changes.
This aspect of assessment can help determine whether further observation or intervention might be beneficial.
Considering the Eye’s Drainage System
The eye’s drainage system regulates fluid and helps maintain intraocular pressure within a healthy range. An assessment of how well fluid flows through the eye can provide information about potential risk factors for glaucoma.
Understanding the eye’s drainage capacity can help inform different treatment approaches, though not every clinic may perform detailed drainage system testing during routine exams.
Additional Considerations
Other factors, such as corneal thickness or blood pressure, may influence risk and eye pressure readings. These elements can be relevant in assessing the likelihood of developing glaucoma or monitoring disease progression over time.
By combining information from eye pressure measurements, optic nerve evaluation, vision assessment, and other factors, a comprehensive exam can provide a broader understanding of eye health and potential glaucoma risk. While each clinic may offer different types of eye assessments, knowing what to expect can help you feel more prepared for a glaucoma evaluation.
Managing Glaucoma
Once glaucoma is diagnosed, the primary goal is to lower eye pressure and prevent further optic nerve damage. The approach to management varies depending on the type of glaucoma, the disease progression, and your overall eye health.
A tailored plan allows your eye doctor to address your specific needs while supporting long-term vision preservation.
Prescription Eye Drops
Prescription eye drops are often the first line of treatment. These medications lower eye pressure by either reducing fluid production in the eye or helping the eye drain excess fluid more effectively.
Consistent use as directed by your eye doctor can slow optic nerve damage and support early treatment outcomes.
Laser Treatment
Laser procedures provide targeted methods to assist with eye pressure management. Two laser surgeries are:
- YAG Laser Iridotomy: Often recommended for angle-closure glaucoma, this procedure creates a small opening in the iris to improve fluid circulation.
- Selective Laser Trabeculoplasty (SLT): Typically used for open-angle glaucoma, SLT targets the drainage system to enhance fluid outflow and help lower eye pressure.
Laser treatment can complement eye drops or, in some cases, serve as a primary intervention, depending on your condition.
Minimally Invasive Glaucoma Surgery (MIGS)
For patients requiring surgical intervention, the clinic offers minimally invasive glaucoma surgery (MIGS), including:
- iStent: A tiny implant placed in the drainage angle to facilitate fluid outflow.
- Hydrus Microstent: Designed to expand the drainage system, assisting with intraocular pressure reduction.
MIGS procedures are designed to support effective fluid drainage and generally offer shorter recovery times than traditional surgeries.
A successful management strategy is guided by your eye doctor and tailored to your individual needs. Factors such as glaucoma type, optic nerve health, eye pressure, and other risk factors influence the recommended treatment options.
Ongoing monitoring through comprehensive eye exams ensures that the treatment plan evolves as your condition progresses.
By combining early detection, consistent monitoring, and a personalised approach, it is possible to slow disease progression, preserve vision, and maintain overall eye health.
Frequently Asked Questions
How often should glaucoma be monitored once diagnosed?
Monitoring frequency depends on the type and severity of glaucoma. Early stages may require check-ups every 6–12 months, while more advanced cases may need closer monitoring to ensure treatment effectiveness and detect changes in optic nerve health.
Can glaucoma be prevented?
While glaucoma cannot always be prevented, early detection, regular glaucoma exams, and consistent monitoring can help reduce the risk of irreversible vision loss. Maintaining overall eye health and managing medical conditions, such as high blood pressure, also supports prevention.
How does a thin cornea affect glaucoma risk?
A thin cornea can influence eye pressure readings and may be associated with a higher risk of developing glaucoma. Your eye doctor may consider corneal thickness when interpreting eye pressure tests and designing a treatment plan.
Can low or high blood pressure affect glaucoma?
Yes. High blood pressure may increase intraocular pressure, while low blood pressure can reduce blood flow to the optic nerve, both of which can contribute to optic nerve damage. Blood pressure management is considered part of overall eye health.
Can cataract surgery affect glaucoma?
In some cases, cataract surgery may help lower eye pressure by improving fluid drainage. Your eye doctor may recommend this procedure as part of a broader treatment plan for certain types of glaucoma.
Conclusion

When detected early, glaucoma treatment can help slow disease progression and support long-term vision.
Regular check-ups, awareness of risk factors, and prompt attention to sudden symptoms are vital components of maintaining eye health. Working closely with your eye doctor allows you to develop a tailored treatment plan that protects your vision.
If you’re due for a comprehensive eye exam or have concerns about eye pressure, optic nerve health, or your risk factors, our experienced eye doctors are here to guide you.
Book a consultation with Armadale Eye Clinic at (03) 9070 5753 to discuss your personalised glaucoma assessment and explore the treatment options available to support your long-term vision. Early evaluation can ensure your eyes receive the attention they deserve.
Note: Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
References
Reddy, N. (2024, February 5). Laser Surgery for Glaucoma: How It Works and What to Expect. GoodRx. Retrieved November 24, 2025, from https://www.goodrx.com/conditions/glaucoma/glaucoma-surgery
Reiff Ellis, R. (2024, December 30). What is Acute Angle Closure Glaucoma? WebMD. Retrieved November 24, 2025, from https://www.webmd.com/eye-health/acute-angle-closure-glaucoma
Tee-Melegrito, R. A. (2023, May 18). What Does Glaucoma Vision Look Like? Medical News Today. Retrieved November 24, 2025, from https://www.medicalnewstoday.com/articles/what-does-glaucoma-vision-look-like
The Healthline Editorial Team. (2025, April 8). What To Know About Glaucoma. Healthline. Retrieved November 24, 2025, from https://www.healthline.com/health/glaucoma







 Overview of High Blood Pressure
Overview of High Blood Pressure Blood Pressure Levels and Eye Health
Blood Pressure Levels and Eye Health What is ocular hypertension?
What is ocular hypertension?

 Deciding whether glaucoma surgery is right for you can feel overwhelming, and that’s perfectly okay. But by learning what happens before and after glaucoma surgery, you’re already on the path to making an informed, confident choice.
Deciding whether glaucoma surgery is right for you can feel overwhelming, and that’s perfectly okay. But by learning what happens before and after glaucoma surgery, you’re already on the path to making an informed, confident choice.
 The Role Of Eye Pressure
The Role Of Eye Pressure Changes In Peripheral Vision
Changes In Peripheral Vision

 People with ocular hypertension usually don’t feel anything. It’s called a “silent” condition because no obvious signs exist. That’s why it’s important to see the eye doctor.
People with ocular hypertension usually don’t feel anything. It’s called a “silent” condition because no obvious signs exist. That’s why it’s important to see the eye doctor. The goal is to lower the eye pressure and
The goal is to lower the eye pressure and Taking care of your eyes is important to
Taking care of your eyes is important to
 Glaucoma is an
Glaucoma is an  Glaucoma hereditary patterns suggest that those with immediate family members who have glaucoma are at a greater risk of developing the condition.
Glaucoma hereditary patterns suggest that those with immediate family members who have glaucoma are at a greater risk of developing the condition. Finding the answer to the common question, “Is glaucoma hereditary?” is essential for those with a family history of the condition.
Finding the answer to the common question, “Is glaucoma hereditary?” is essential for those with a family history of the condition.
 Primary open-angle glaucoma is a prevalent type of glaucoma. It occurs when the drainage angle created by the cornea and iris stays open, but the trabecular meshwork is partially obstructed. This causes a gradual increase in eye pressure, leading to optic nerve damage.
Primary open-angle glaucoma is a prevalent type of glaucoma. It occurs when the drainage angle created by the cornea and iris stays open, but the trabecular meshwork is partially obstructed. This causes a gradual increase in eye pressure, leading to optic nerve damage. Increased intraocular pressure (IOP) is the most significant risk factor for glaucoma, particularly for primary open-angle glaucoma.
Increased intraocular pressure (IOP) is the most significant risk factor for glaucoma, particularly for primary open-angle glaucoma.  Understanding the types of glaucoma, recognising the signs, identifying the reasons, and knowing how to manage this condition can help preserve vision and slow down, if not prevent, significant vision loss. Comprehensive eye exams, early detection, and appropriate management plans are key to managing glaucoma effectively.
Understanding the types of glaucoma, recognising the signs, identifying the reasons, and knowing how to manage this condition can help preserve vision and slow down, if not prevent, significant vision loss. Comprehensive eye exams, early detection, and appropriate management plans are key to managing glaucoma effectively.


